The urologic care of children with spina bifida has changed in recent years. In the past, children with spina bifida often got urinary tract infections that caused serious kidney disease. Fortunately, this is no longer the case. We now try to prevent kidney disease. We also have made great progress in helping children with spina bifida become dry.
What is the urinary tract system?
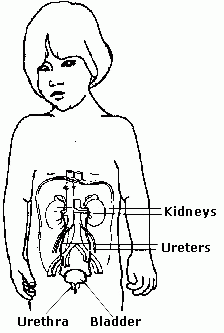
The urinary tract system consists of two kidneys, two ureters, the bladder, the sphincter muscle, which controls the flow of urine and the urethra, which brings the urine from the bladder to the outside world.
The kidneys filter the blood and make urine. Urine goes from the kidneys to the bladder through tubes called the ureters. Where the ureters and the bladder join, there are one-way valves that stop the urine from going backwards into the kidneys. The bladder holds the urine, and then releases it through the urethra every few hours. Normally, as urine fills the bladder, it stretches to hold more and more urine at a low bladder pressure. When the bladder becomes full, a message is sent to the brain. Signals from the brain then tell the sphincter muscle to relax, and the bladder muscle to contract at the same time, so the bladder can empty. Normally, a person can wait until it is the right time to empty the bladder.
How does spina bifida affect the kidneys and bladder?
Most infants with spina bifida are born with kidneys that work well, although this can change. Most children with spina bifida have what is called a neurogenic bladder. In a neurogenic bladder, the nerves going from the spinal cord to the brain do not work properly. The child may not be aware that the bladder is full and often cannot empty the bladder well. Also, the sphincter muscle may not work. It may either stay relaxed or not relax when the bladder is contracting. If the bladder doesn't empty well, it can cause damage to the kidneys and/or lead to urinary tract infections. Only about 5 percent of children with spina bifida are able to empty their bladders without help.
Goals of urological management
- To make sure the kidneys are working well and prevent damage
- To help the child to empty the bladder
- To help the child stay dry
What tests will be done to assess your child's urinary tract?
Ongoing assessment and monitoring of the urinary tract system will be an important part of your child's care. This may include any of the following tests:
- Urinalysis and urine culture: To check for infection
- Blood tests including creatinine and BUN (blood urea nitrogen): To check how well the kidneys are working
- Renal/bladder ultrasound: This is a test done in the X-ray Department that checks the size and shape of the kidneys and bladder, as well as checking for other abnormalities.
- VCUG (voiding cystourethrogram): This is a test done in the X-ray department to check for reflux, which is when the urine flows backwards from bladder to the kidneys. It also shows the shape of the bladder and urethra, and how well the bladder empties.
- Urodynamic tests: This is a special study that shows how the bladder works, including:
- How much urine the bladder will hold
- At what pressures the bladder fills, stores and empties urine
- How well the bladder empties
- How well the bladder and sphincter muscle work together
- If reflux is present, information from this test helps to show which children may be at risk for developing problems. It is also helpful in keeping track of how the child's bladder is responding to treatment.
- Renal scans: These scans provide information on:
- How well the kidneys work
- If there is a problem with the drainage of urine from the kidneys to the bladder
- If there are scars on the kidneys (showing past infection) or other changes indicating current infection
What urological problems are common in children with spina bifida?
- Urinary tract infections
- Vesico-ureteral reflux: This is when the urine backs up from the bladder through the ureters to the kidneys. This can be caused by high pressures in the bladder. Reflux can cause kidney damage because infection can spread from the bladder to the kidneys.
- Hydronephrosis: Swelling of the kidney from the backup of urine. This can be caused by high bladder pressures.
- Incontinence: The child is unable to stay dry. This can cause both physical and social problems.
Why do these problems occur?
Due to nerve damage, the bladder and sphincter muscle may not work properly. The bladder is supposed to fill and store urine at low pressure and empty every few hours. Both of these may be affected.
Problems with filling and storage
- The bladder is not able to keep pressures low as it fills with urine. High bladder pressures can hurt the kidney.
- The bladder is not able to hold as much urine as it should.
Problems with bladder emptying
- Leaking of urine can occur when bladder pressures are too high and the bladder overpowers the sphincter muscle. Leaking may also occur even with normal bladder pressures if the sphincter muscle is very relaxed and doesn't tighten when it should.
- The bladder may not empty all the way. This may happen because the bladder isn't strong enough, or because the sphincter muscle doesn't relax when the bladder contracts.
What will be done to keep your child's urinary tract healthy?
Closely checking the child's urinary tract is necessary. At different ages, various suggestions may be made. These include:
- Clean intermittent catheterization: A procedure to empty the bladder by inserting a soft, flexible tube called a catheter into the bladder to drain the urine. This helps prevent infections, reduces bladder pressures, and helps the child to become dry.
- Medications are given to:
- Prevent and treat infection. These are called antibiotics.
- Relax the bladder so it may hold more urine at low pressures. These are called anticholinergics and include ditropan, levsin, or levsinex/levbid.
- Help prevent leaking.
- Surgery: Sometimes surgery is needed when medicines and clean intermittent catheterization do not work well enough. There are several procedures used, depending on what type of problem needs to be treated. Some surgical procedures are temporary; some are permanent. Surgery may be done to treat reflux, to enlarge the bladder, to improve sphincter function, or to provide emptying of the bladder through other ways than the urethra.
Ongoing assessment and management by age
Newborns
Several tests are done shortly after birth to learn about the baby's urinary tract system. Baseline studies include:
- Urinalysis or urine culture
- BUN and creatinine
- Post void residual. This is the amount of urine left in the bladder after the baby has wet a diaper. This is done by catheterizing the baby and measuring the amount of urine left in the bladder.
- Renal or bladder ultrasound to check for physical abnormalities that would put the baby at risk for problems
- Urodynamic studies to check bladder pressures and emptying ability is usually done during the first month of life
Your infant's urologist will make suggestions based on what is learned from the various tests. In general:
- If no reflux or swelling of the kidney is present, bladder pressures are low, and there is not a large amount of urine left in the bladder, nothing special may be needed and the baby may wet normally in the diapers.
- If reflux is present, the baby may be started on clean intermittent catheterization and a daily low dose of an antibiotic to prevent infections.
- If the bladder pressures are high, clean intermittent catheterization is started. Anticholinergic medications may also be started to help relax the bladder and lower pressures.
- If medicine and clean intermittent catheterization are not helping enough, or if it is too hard for the parents catheterize their infant on a regular basis, surgery may be needed.
Infants
Close monitoring of the infant's urinary tract is done during the first year of life. Generally renal ultrasounds and/or urodynamic studies are done every 3 to 6 months. This is because there can be changes in how the bladder works as the baby grows and the nerves and spinal cord develop. The tests also show how the infant is responding to his current care plan. A catheterized urine culture should be done any time the baby may have a urinary tract infection. Symptoms of infection in a baby include fever, fussiness, and not eating well.
Toddlers
Continued close monitoring is important. Renal ultrasounds are obtained every 3 to 6 months and urodynamic studies every 6 months. A catheterized urine culture should be done if the child shows signs of infection.
Preschoolers
Renal ultrasounds and urodynamic studies are done every 6 to 12 months. Clean intermittent catheterization with or without medicine may be started to keep the child dry. A catheterized urine culture should be done if the child shows symptoms such as; fever, back pain, foul smelling urine, or increased wetting.
School-age children
Yearly renal ultrasound and urodynamic studies are done as indicated. Catheterized urine cultures should be done if the child shows symptoms of a urinary tract infection. The child may begin self-clean intermittent catheterization if he feels ready.
Adolescents
Yearly renal ultrasound and other tests will be done as needed. Urine cultures should be done any time there are symptoms of infection. By this time, adolescents should know the signs and symptoms of urinary tract infection, how to take their medicines, and how to catheterize themselves. Sexual function and expectations should be discussed.
Page reviewed on: Aug 16, 2004